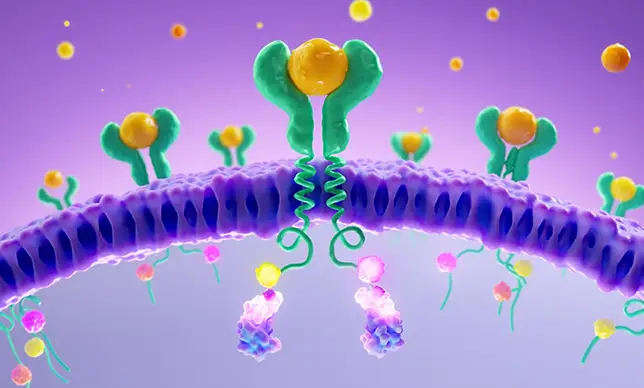
HS is more than skin deep. It’s driven by chronic inflammation.
HS involves multiple cell types and cytokines, several of which are mediated by JAK-STAT signaling.1–3
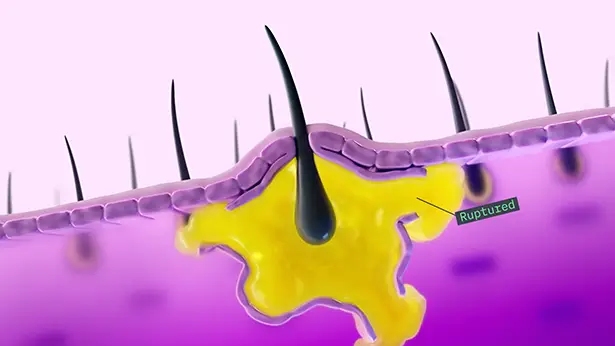
Inflammation begins under the skin when a hair follicle becomes occluded and dilated, then ruptures, releasing cellular debris into the dermis.4
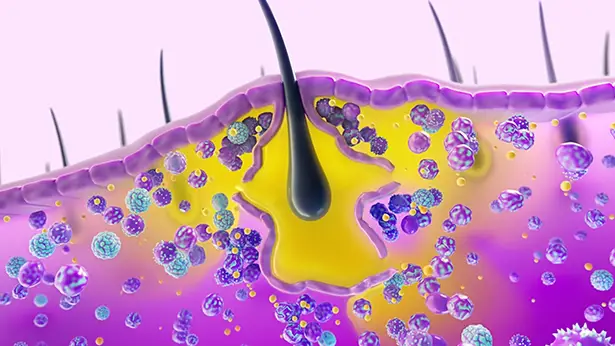
This triggers key inflammatory pathways to become activated. Rather than healing the tissue, a complex immune response becomes pathologic in HS, setting off a harmful inflammatory cascade that can lead to the formation of additional nodules, abscesses, and draining tunnels in the skin.2

Many different cytokines are involved in HS, directing the immune response by sending signals inside various cell types, including immune cells, keratinocytes, fibroblasts, and endothelial cells.1,2
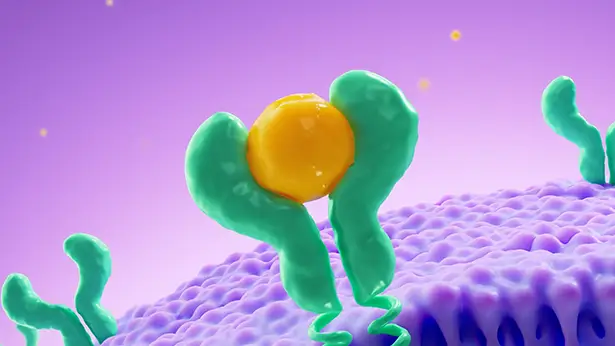
Several cytokines rely on the JAK-STAT pathway to direct an immune response.5
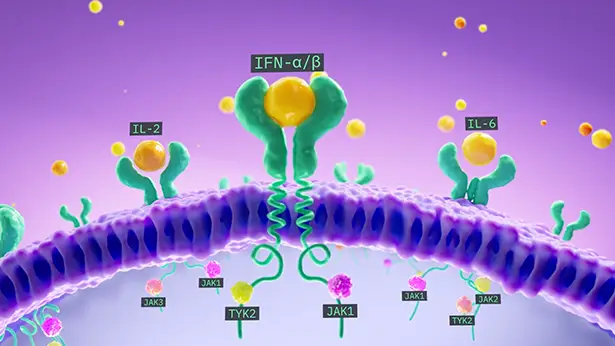
The JAK enzymes are key for communication between cytokines and the cell nucleus. Their signaling amplifies the inflammatory immune response. JAK1 is activated by a wide range of cytokines, which makes it an important factor in HS pathophysiology.5,6
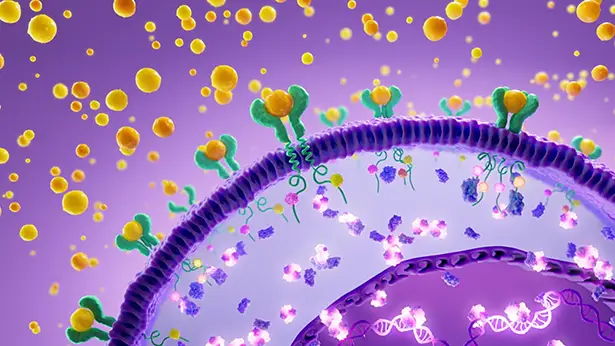
Understanding the role of the JAK-STAT pathway, including JAK1, in mediating the inflammatory cascade of HS is important.5,6
For people with HS, this immune signaling becomes an overpowering inflammatory cascade that is a main driver of HS symptoms.2,6

“Staying optimistic on my side has become much easier with all of these new therapies that we now have available.”
HS, hidradenitis suppurativa; JAK1, Janus kinase 1; JAK-STAT, Janus kinase-signal transducer and activator of transcription.
REFERENCES: 1. Sabat R, Alavi A, Wolk K, et al. Hidradenitis suppurativa. Lancet. 2025;405(10476):420-438. doi:10.1016/S0140-6736(24)02475-9 2. Wolk K, Join-Lambert O, Sabat R. Aetiology and pathogenesis of hidradenitis suppurativa. Br J Dermatol. 2020;183(6):999-1010. doi:10.1111/bjd.19556 3. Gadina M, Johnson C, Schwartz D, et al. Translational and clinical advances in JAK-STAT biology: The present and future of jakinibs. J Leukoc Biol. 2018;104(3):499-514. doi:10.1002/JLB.5RI0218-084R 4. Saunte DML, Jemec GBE. Hidradenitis suppurativa: advances in diagnosis and treatment. JAMA. 2017;318(20):2019-2032. doi:10.1001/jama.2017.16691 5. Rumberger BE, Boarder EL, Owens SL, Howell MD. Transcriptomic analysis of hidradenitis suppurativa skin suggests roles for multiple inflammatory pathways in disease pathogenesis. Inflamm Res. 2020;69(10):967-973. doi:10.1007/s00011-020-01381-7 6. Krueger JG, Frew J, Jemec GBE, et al. Hidradenitis suppurativa: new insights into disease mechanisms and an evolving treatment landscape. Br J Dermatol. 2024;190(2):149-162. doi:10.1093/bjd/ljad345